Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Menopause symptoms vary. The natural strategies described are for symptom management, not medical treatment. Always consult your healthcare provider about managing menopause symptoms, including hormone therapy or other interventions.
📞 Before you read: If you experience severe insomnia (less than 4 hours of sleep per night, multiple nights per week) or if your sleep problems are accompanied by depression, anxiety, or thoughts of self‑harm, see a doctor immediately. Natural strategies are complementary tools – not replacements for professional medical care.
“My body used to know when to sleep. Now it seems confused.”
That’s what my friend Diane whispered to me over coffee last week. She’s 52, in perimenopause, and she’s exhausted.
She falls asleep fine. But at 2 AM, she’s wide awake. Her mind starts racing. Then she lies there until dawn.
“I feel like my internal clock is broken,” she said.
I smiled and handed her a printout – the same one I’m sharing with you.
This article is for anyone who:
- Used to sleep like a baby but now wakes up at the same weird hour every night
- Feels tired during the day but wired when the head hits the pillow
- Has tried all the sleep hygiene tips yet still tosses and turns
- Wants to understand the deeper science behind menopause sleep disruption
The short answer: Declining estrogen during menopause can disrupt your master body clock – the suprachiasmatic nucleus (SCN) – causing your sleep‑wake cycle to go haywire.
This means you can: Using targeted light exposure, meal timing, and gentle melatonin support can help reset your internal clock naturally. Let’s explore the science and simple, effective strategies to restore your circadian rhythm.
Your Body’s Incredibly Precise Timekeeper: An Introduction
Think of your body as having a master conductor – a tiny region in your brain called the hypothalamic suprachiasmatic nuclei (SCN). This conductor directs a symphony of daily rhythms: when you feel sleepy, when you wake up, when you feel hungry, and even when your body temperature rises and falls.
But what happens when the conductor loses its sheet music? The music becomes chaotic.
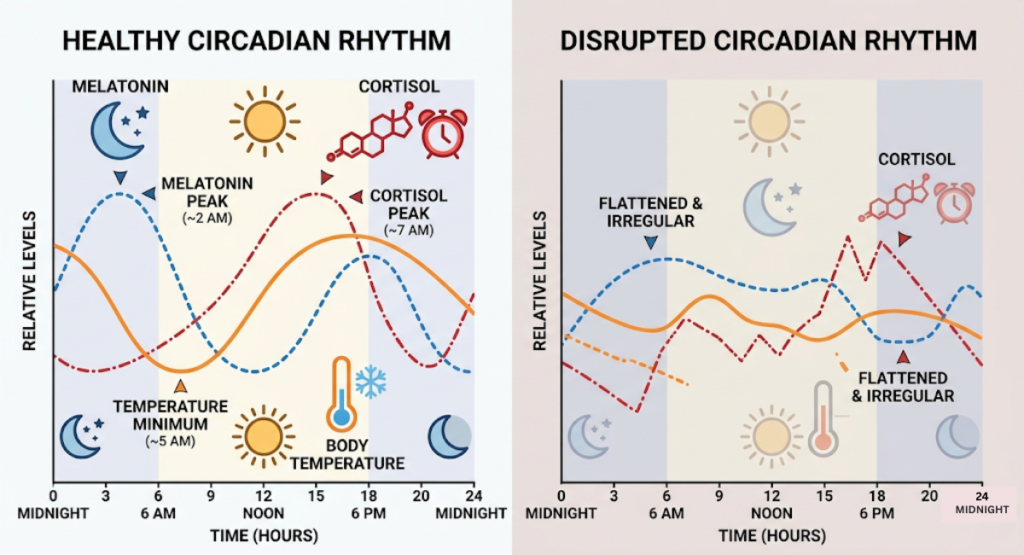
Your SCN relies on signals to stay on track. The most powerful signal is light. When morning light hits your eyes, it tells your SCN to suppress melatonin, the hormone that makes you feel drowsy. As night falls, darkness allows melatonin to rise, preparing you for sleep.

This beautifully orchestrated system, however, becomes much more fragile during the menopausal transition. Research confirms that menopausal changes in estrogen levels can directly disrupt melatonin synthesis and secretion, which contributes to the sleep disturbances that are so common during this phase of life.
The Menopause‑Circadian Rhythm Cascade: What’s Really Happening
Several interconnected changes explain the frustrating sleep issues of menopause.
1. The “Phase Advance” (Your Clock Runs Early)
In perimenopause, the body’s circadian phase shifts earlier. This means your body starts preparing for sleep hours before it used to, and you also wake up earlier – often around 3 AM to 4 AM. You may feel tired at 8 PM but then find yourself staring at the ceiling at 3 AM with a racing mind.
2. Blunted Melatonin (The Sleep Signal Weakens)
Estrogen helps regulate melatonin secretion. As estrogen drops, the melatonin signal can become smaller and less distinct. It is as if someone turned down the volume on your natural sleep cue – you still get the signal, but it is no longer powerful enough to keep you asleep. Consequently, your sleep becomes lighter, more fragmented, and less restorative.
3. Increased Sensitivity to Disruption (The System Becomes Fragile)
Your SCN becomes more vulnerable to things that never used to bother you. A small amount of light at night, a slightly late dinner, or a stressful day can now throw your entire rhythm off balance for days or even weeks.
4. Hot Flashes on a Schedule (Circadian Periodicity)
Hot flashes are not random. They follow a distinct circadian pattern. Postmenopausal hot flashes occur more frequently when core body temperature is naturally at its highest – typically in the late afternoon and evening. For women who experience frequent hot flashes, the peak often occurs around 6:25 PM. This predictable rhythm means that part of your sleep disruption is a biological event connected directly to your altered body clock.
The Domino Effect: From a Disrupted Clock to a Disrupted Life
Once your master clock starts to malfunction, it creates a cascade of problems. Over time, this internal misalignment leads to insomnia, mood changes, and altered energy levels. In other words, the fatigue and brain fog you are experiencing are very real and have a solid scientific basis. You are not imagining it, and you are not “just getting older.”
How to Reset Your Menopausal Circadian Rhythm Naturally

🏆 1. Bright Light Therapy (The Most Powerful Tool)
Recent clinical trials show that resetting the circadian rhythm through bright light exposure directly improves mood and sleep function in menopause. Sleep‑light interventions that shift melatonin rhythms earlier in the night significantly improve perimenopausal and postmenopausal depression.
Your action plan: Use a 10,000‑lux light box for 20–30 minutes within 30 minutes of waking up. This gives your body clock a clear, strong signal that the day has started. Place the light box at a 45‑degree angle, about 2 feet away from your face, while you read emails, eat breakfast, or check the news.

Placement: Inside the bright light therapy section
Caption: “A 10,000‑lux light box used for 20–30 minutes each morning can help advance your circadian phase and improve sleep quality.”
🌿 2. Strategic Melatonin Support
Melatonin works best for circadian rhythm‑related difficulties, such as delayed sleep onset or irregular sleep schedules. For menopausal women, who often produce a blunted melatonin signal, a low‑dose supplement can help consolidate sleep.
Your action plan: Take 0.5–3 mg of melatonin 60–90 minutes before your desired bedtime. Use it for short periods (2–4 weeks) alongside other rhythm‑resetting strategies rather than as a long‑term fix.
🧠 3. Cognitive Behavioral Therapy for Insomnia (CBT‑I)
CBT‑I is a highly effective non‑pharmacological intervention for improving sleep quality and reducing insomnia severity in menopausal women. It works by breaking the vicious cycle of anxiety about sleep and the poor sleep itself. It is even more powerful when combined with circadian rhythm therapy.
Your action plan: Work with a therapist or use a reputable online program. Core techniques include: (a) Stimulus control – get out of bed if you can’t sleep, (b) Sleep restriction – limit time in bed to actual sleep time, and (c) Cognitive restructuring – challenge unhelpful thoughts like “I’ll never sleep again.”
😌 4. Mindfulness for 2‑AM Wake‑Ups
Mindfulness has shown great promise for menopausal insomnia. The key is to short‑circuit the anxiety spiral when you wake up at 3 AM. Instead of engaging with racing thoughts, bring your attention to the physical sensation of your breath in the lower belly.
Your action plan: When you wake up at night and feel your mind start to race, practice this simple breathing awareness for 3 to 5 minutes. Even if you don’t fall back asleep, you break the cycle of sleep anxiety.
💪 5. Light‑Intensity Morning Exercise
Morning exercise – especially a brisk walk – is one of the most underrated tools for menopause sleep. It signals daytime activity to your body clock, stabilizes your core body temperature rhythm, and reduces anxiety.
Your action plan: Take a 20‑30 minute brisk walk within 2 hours of waking. Try to get sunshine exposure at the same time for an even better effect.
[Image: Woman walking briskly in morning light – alt text: “Morning walk routine for menopause sleep and circadian health”]
Placement: Inside the morning exercise section
Caption: “A 20‑minute brisk walk in the morning sun is free exercise plus free light therapy – a powerful combination for resetting your body clock.”
🕰️ 6. Time Your Meals
Your eating schedule acts as a secondary time cue (called a “zeitgeber”). Erratic meal times confuse your SCN, while regular, predictable meals strengthen your rhythm.
Your action plan: Finish your last meal at least 2‑3 hours before bed. Eat your breakfast, lunch, and dinner at roughly the same times each day.
Myth vs. Fact: Circadian Rhythm & Menopause
| Myth | Fact |
|---|---|
| “You just have to accept poor sleep as a normal part of menopause.” | False. Sleep disruption is common but not inevitable. Targeted interventions like bright light therapy and CBT‑I can be highly effective. |
| “Taking melatonin is the same as getting good sleep.” | False. Melatonin is a timing signal, not a sleeping pill. It helps reset your body clock but does not force sleep. Combine it with good sleep hygiene. |
| “You should stay in bed and keep trying to fall back asleep.” | False. Lying awake for more than 20 minutes trains your brain to associate your bed with wakefulness and frustration. Get up, move to a dark room, and return only when you feel sleepy. |
| “Hot flashes are random and unpredictable.” | Not entirely. Hot flashes follow a circadian rhythm. Many women have a peak in late afternoon and a secondary peak in the early morning hours. |
Common Mistakes to Avoid
- Relying only on melatonin – Taking melatonin without fixing light exposure and meal timing is like using a band‑aid on a broken bone. It might help temporarily, but it won’t solve the underlying rhythm disruption.
- Getting bright light at the wrong time – Morning light advances your rhythm, helping with early morning awakenings. Evening bright light delays your rhythm, making it harder to fall asleep. Reduce all screens and bright overhead lights 90 minutes before bed.
- Irregular sleep‑wake schedule – The most important anchor for your SCN is a consistent wake time. Sleeping in on weekends can undo a week’s worth of rhythm‑setting work.
- Ignoring other symptoms – Daytime fatigue, brain fog, and mood changes are not separate issues. They are downstream effects of a disrupted circadian rhythm. Fixing your sleep will cascade into daytime improvements.
Real‑Life Examples: Women Who Reset Their Clocks
Margaret, 56 (post‑menopause): “I was convinced that I had chronic, untreatable insomnia. I would wake up at 3 AM every night and never fall back asleep. My therapist introduced me to bright light therapy. Within two weeks, my wake‑up time shifted to 5 AM. I still wake up, but now I can fall back asleep within 10 minutes.”

Linda, 50 (perimenopause): “My big issue was falling asleep. I would lie in bed for hours, my mind spinning. Melatonin alone did nothing. However, when I added a 7 PM technology curfew and a 15‑minute mindfulness practice, everything changed. I now fall asleep within 20 minutes.”
🚨 When to See a Doctor (Not Just Try Natural Remedies)
If you experience any of the following, see a doctor:
- Less than 4 hours of sleep per night, most nights – This can impair immune function and increase cardiovascular risk.
- Loud snoring or gasping during sleep – Possible sleep apnea, which is common in menopause and often underdiagnosed.
- Depressed mood or thoughts of self‑harm – Menopause can worsen mood disorders. Get help immediately.
- Night sweats that soak through bedding every night – Could indicate an underlying medical condition.
- Daytime sleepiness affecting driving or work – Falls and accidents are real risks.
Persistent insomnia symptoms are associated with a 71% increased incidence of cardiovascular events. Therefore, don’t ignore your sleep problems.
Frequently Asked Questions
How does estrogen affect circadian rhythm?
Estrogen helps regulate the timing and strength of melatonin secretion. It also affects how your SCN responds to light. As estrogen drops during perimenopause, the master clock becomes weaker and more easily disrupted.
Can I use a light box if I have eye problems?
Consult your doctor first. People with certain eye conditions (macular degeneration, diabetic retinopathy, glaucoma) should be cautious with bright light therapy.
What’s the best time to take melatonin for menopause?
For early morning awakenings (waking at 3‑4 AM), take a low‑dose (0.5‑1 mg) sustained‑release melatonin at bedtime. For difficulty falling asleep, take 1‑3 mg immediate‑release melatonin 60‑90 minutes before bed. Always start with the lowest effective dose.
How long does it take to reset my circadian rhythm?
With consistent daily practices (morning light, fixed wake time, evening dim light), most women see noticeable improvement within 7‑14 days. Full stabilization of the sleep‑wake cycle typically takes 4‑8 weeks.
Your 4‑Step Circadian Rhythm Reset Action Plan (Printable Checklist)
| Step | Action | Frequency |
|---|---|---|
| 1 | Get 15‑30 minutes of morning sunlight or 10,000‑lux light box | Within 30 minutes of waking |
| 2 | Take a 20‑30 minute brisk morning walk | 5‑7 days per week |
| 3 | Eliminate screens 90 minutes before bed | Every night |
| 4 | Practice mindfulness for 5‑10 minutes at bedtime | Every night |
[Image: Printable checklist for circadian rhythm reset – alt text: “4‑step action plan for resetting menopause circadian rhythm”]
Placement: After the action plan
Caption: “Consistency is more important than intensity. Start with just step 1 for one week, then gradually add steps 2‑4.”
My Final Verdict
The science is clear: menopause directly affects your internal body clock. The good news is that your clock can be reset. It responds powerfully to the right cues – morning light, consistent sleep and meal times, and targeted behavioral strategies like CBT‑I and mindfulness.
Be patient with yourself. It took months or years for this rhythm disruption to develop, and it may take several weeks to restore it. Celebrate small wins: one more hour of sleep, one less nighttime awakening, one morning with clear thinking instead of brain fog.
[CTA] Ready to reset your body clock? [Click here] to see my recommended light therapy devices and sleep trackers.
[Bonus CTA] Download my free PDF: “Menopause Circadian Rhythm Reset Checklist” – no email required.
Medical References (Clickable Links)
- A prospective study to investigate circadian rhythms as health indicator in women’s aging – npj Women‘s Health, 2025
- Circadian rhythm disruptions in menopause: symptoms and interventions – npj Women’s Health, 2025
- Changes in nocturnal melatonin secretion in perimenopausal women – Journal of Pineal Research, 2000
- Systematic review of nonpharmacological interventions for menopausal women – Wiley, 2024
- Circadian rhythm of hot flashes in menopausal women – Journal of Clinical Endocrinology and Metabolism, 1995
- Sleep and Light Intervention (SALI) for Menopausal Mood Dysfunction – NIH Clinical Trial, 2024
- Effectiveness of nonpharmacological interventions for menopause-related insomnia – Maturitas, 2025 – DOI: 10.1016/j.maturitas.2025.108713
Medical Disclaimer (repeated): This article is for informational purposes only. The natural strategies described are for symptom management, not medical treatment. Always consult your healthcare provider about managing menopause symptoms. Do not stop prescribed medications without consulting your doctor.
Last updated: April, 2026
Published: April, 2026











