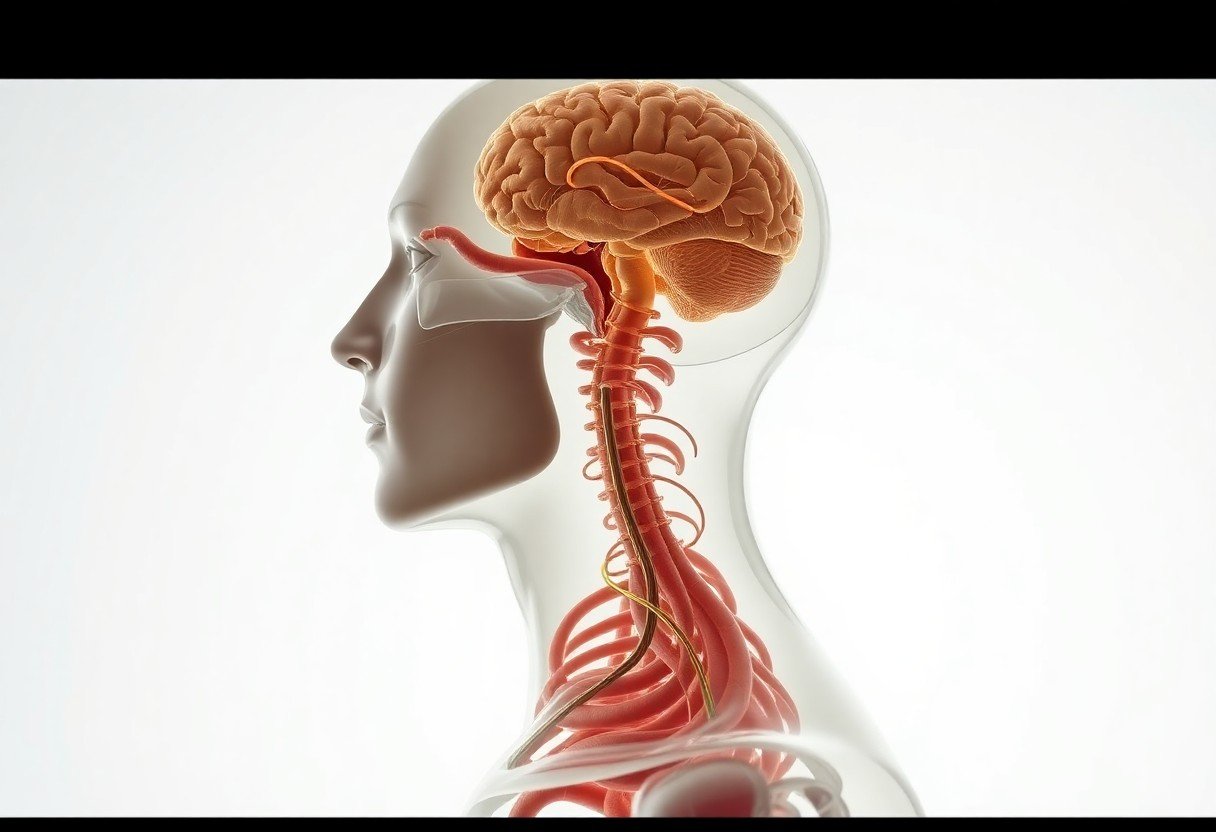
Mood connects your gut and brain: your digestion shapes neurotransmitters and immune signals, so you may feel anxious or calm. Gut inflammation can worsen anxiety, while restoring healthy microbes often improves mood via serotonin and the vagus nerve.
The Biological Infrastructure: The Vagus Nerve and the Enteric System
This network of vagal pathways and the enteric nervous system channels gut signals that shape your mood and anxiety, with bi-directional communication meaning gut disturbances can aggravate or relieve mental symptoms depending on immune and neural states.
The Enteric Nervous System: Understanding the “Second Brain”
Your enteric nervous system houses about 100 million neurons that regulate digestion and send chemical and neural cues to the brain, so gut dysfunction can trigger or intensify anxiety.
The Vagus Nerve as a Bi-directional Communication Highway
Vagus nerve traffic moves both directions between gut and brain, so gut inflammation can heighten anxiety, while targeted vagal stimulation can reduce stress and improve mood.
You can trace vagal afferents carrying microbial metabolites, stretch signals, and immune mediators to emotional brain centers, and vagal efferents then alter gut motility and inflammation; chronic cytokine release from the gut may sustain anxiety by shifting neurotransmitter balance, whereas practices that boost vagal tone like deep breathing and cold exposure can lower stress and aid recovery.
Neurochemical Synthesis within the Gut Microbiome
Microbial communities in your gut synthesize neurotransmitters and precursors that shape mood and anxiety; they influence brain signaling via the vagus nerve, immune activation, and metabolic routes, with serotonin, GABA, and dopamine particularly impactful.
Microbial Production of Serotonin, GABA, and Dopamine
Certain gut bacteria produce or modulate serotonin, GABA, and dopamine, so shifts in your microbiome can lower mood-regulating signals and increase anxiety risk by altering vagal and immune communication to the brain.
Short-Chain Fatty Acids and Their Influence on Brain Function
Butyrate and other short-chain fatty acids generated from fiber fermentation reduce gut inflammation, support the blood-brain barrier, and modulate neurotransmitter synthesis, often improving mood and reducing anxiety when your microbiome produces enough.
When your diet supplies fermentable fiber, bacteria convert it into acetate, propionate, and butyrate that act on enteroendocrine cells, immune pathways, and microglia to lower neuroinflammation and regulate gene expression via histone deacetylase inhibition; low SCFA levels are linked to increased inflammation and higher rates of depression in animal and human studies, while boosting fiber and prebiotics raises SCFAs and supports the blood-brain barrier.
The Role of Intestinal Permeability and Systemic Inflammation
Intestinal permeability permits microbial fragments and toxins into your bloodstream, provoking systemic inflammation that shifts neurotransmitter systems and can worsen mood regulation; chronic immune activation then feeds anxiety via neuroimmune pathways.
Leaky Gut Syndrome and the Triggering of Immune Responses
Leaky gut allows bacterial endotoxins to enter your circulation, triggering immune responses and sustained cytokine release that may amplify anxiety; chronic inflammation increases threat to mood stability.
Pro-inflammatory Cytokines and Their Link to Anxiety Disorders
Pro-inflammatory cytokines such as IL-6 and TNF-α signal to your brain, alter serotonin and GABA pathways, and raise anxiety vulnerability.
Chronic exposure to elevated cytokines can disrupt the blood-brain barrier and provoke microglial activation, producing neuronal inflammation that changes how you process fear and stress; immune signaling alters serotonin synthesis and HPA axis reactivity, so you may experience persistent anxiety and cognitive fog, while interventions like a whole-food anti-inflammatory diet, clinically supported probiotics, adequate sleep and regular exercise can lower cytokine levels and improve your mood.
The Hypothalamic-Pituitary-Adrenal (HPA) Axis and Stress
HPA signaling shapes how you respond to threats, releasing cortisol that alters appetite, inflammation, and gut permeability; these shifts change microbial balance and feed back to your brain, influencing mood and anxiety. Watch for chronic cortisol patterns that can drive persistent anxiety and digestive instability.
Impact of Chronic Cortisol Elevation on Microbiota Composition
Sustained cortisol exposure shifts your gut environment, reducing beneficial bacteria and increasing inflammation-associated strains; these changes can undermine digestion and raise anxiety risk by altering neurotransmitter precursors and mucosal defenses.
The Reciprocal Relationship Between Digestive Distress and Psychological Stress
Digestive discomfort heightens your stress responses, and stress worsens gut symptoms, creating a self-perpetuating cycle that increases anxiety and prolongs digestive dysfunction.
You can experience amplified gut pain and altered motility as stress increases cytokines and vagal signaling, while microbiota shifts change metabolites like short-chain fatty acids and tryptophan availability, influencing serotonin and immune tone. Persistent interaction creates a dangerous chronic cycle that sustains anxiety and gut dysfunction, and targeted interventions such as dietary change, probiotics, and stress-management practices often produce measurable improvements in both mood and digestion.

Nutritional Interventions for Emotional Well-being
You can use targeted nutrition to modulate gut signals that influence mood and anxiety, prioritizing fiber, omega-3s and polyphenol-rich foods to support neurotransmitter synthesis and reduce gut inflammation, which sustains microbiome balance and steadier emotional states.
Therapeutic Potential of Psychobiotics and Fermented Foods
Psychobiotics-specific probiotic strains and fermented foods-can shift microbial activity and produce neuroactive metabolites that ease anxiety; include kefir, yogurt and sauerkraut alongside clinically tested strains to support GABA and serotonin pathways and calmer mood.
The Mediterranean Diet as a Framework for Mental Health
Adopt a Mediterranean-style eating pattern rich in vegetables, whole grains, legumes, olive oil and oily fish to lower inflammation and nourish beneficial microbes, promoting more stable mood through sustained omega-3s and polyphenols.
Research indicates you see reductions in depressive and anxiety symptoms when following Mediterranean patterns, driven by combined effects of anti-inflammatory fats, fiber-driven microbial metabolites and antioxidants; prioritize oily fish twice weekly, extra-virgin olive oil and abundant plant foods while limiting red and processed meats for clearer mental-health benefits.
Identifying Disruptive Dietary Triggers and Ultra-Processed Foods
Recognize that ultra-processed foods, high sugar and industrial additives can provoke inflammation, dysbiosis and increased anxiety; cutting back on packaged snacks, sodas and ready meals supports gut stability and reduces the chance of mood dysregulation.
Practical steps you can take include reading labels for emulsifiers, artificial sweeteners, and high-fructose corn syrup, swapping processed items for whole-food alternatives, and tracking mood responses to identify personal dietary triggers that worsen anxiety or low mood.
Clinical Implications and Future Frontiers in Psychiatry
Clinical teams increasingly view the gut as a target; you should expect dietary interventions, microbiome profiling, and psychobiotic trials to inform treatment plans – read more at You are what you eat: Diet may affect your mood and brain …, and watch for both promising benefits and safety concerns in practice.
Personalized Nutrition and Microbiome Mapping
You can pursue microbiome mapping and tailored diets to reduce anxiety risk factors, with clinicians using sequencing to match interventions; early studies suggest targeted fiber, probiotics, and anti-inflammatory diets may yield measurable mood improvements.
Emerging Research in Fecal Microbiota Transplantation for Mood Regulation
Research shows that fecal microbiota transplantation (FMT) can alter behavior in animal models and preliminary human pilots report mood shifts, but you must weigh infection risks and regulatory hurdles before clinical use.
Trials are now standardizing donor screening, delivery routes, and psychiatric outcome measures so you can better assess FMT’s role; early case series report promising symptomatic reductions, yet you face serious risks including pathogen transmission, immune reactions, and unpredictable microbiome shifts, so FMT should remain an experimental option within controlled studies until larger randomized trials define long-term safety and efficacy.
Summing up
You can influence mood and anxiety by supporting gut health: balanced diet, probiotics, regular sleep and stress management reshape microbiota and gut signaling to improve neurotransmitter balance and emotional resilience.
FAQ
Q: What is the gut-brain axis?
A: The gut-brain axis is the bidirectional communication network linking the gastrointestinal tract and the central nervous system. It operates through neural pathways (particularly the vagus nerve), endocrine signals (hormones), immune mediators (cytokines), and microbial metabolites such as short-chain fatty acids. Gut microbes also synthesize or influence neurotransmitters and their precursors, which can alter brain function, stress responses, and behavior.
Q: How does digestion and gut health affect mood and anxiety?
A: Gut microbes influence the production and availability of neurotransmitters like serotonin, GABA, and dopamine precursors, which play direct roles in mood regulation. Disrupted digestion or increased intestinal permeability can trigger systemic inflammation and activate the hypothalamic-pituitary-adrenal (HPA) axis, elevating stress hormones that worsen anxiety. Sensory and chemical signals from the gut travel via the vagus nerve to brain regions that control emotion, and metabolic products from microbes can modulate neuronal signaling and immune tone, shaping anxiety and mood over time.
Q: Which dietary changes support better mental well-being through the gut?
A: A diet rich in fiber, vegetables, fruits, whole grains, legumes, and oily fish supports microbial diversity and promotes production of beneficial metabolites. Fermented foods and prebiotic-rich items (for example yogurt, kefir, sauerkraut, garlic, onions, bananas) provide live microbes or substrates that feed helpful strains. Reducing highly processed foods, excess added sugars, and heavy alcohol intake lowers inflammatory stimuli that can harm mood. Regular meal timing, adequate sleep, and physical activity also shape the microbiome in ways that support emotional health.
Q: Can probiotics or supplements treat anxiety?
A: Evidence for probiotics treating anxiety is mixed and strain-specific. Some randomized trials report modest reductions in anxiety symptoms with particular strains or combinations (for example Lactobacillus helveticus R0052 plus Bifidobacterium longum R0175, and select Bifidobacterium strains), while other studies show no effect. Probiotics are best considered as adjuncts to proven therapies such as cognitive behavioral therapy or prescribed medications rather than primary treatments. Safety is generally good for healthy adults, but people with severe illness or compromised immunity should consult a clinician before starting supplements.
Q: How long does it take for gut-focused changes to affect mood and anxiety?
A: Short-term shifts in microbial metabolites and gut signaling can occur within days of dietary change, but noticeable improvements in mood or anxiety commonly require several weeks to months of consistent intervention. Magnitude and timing of change depend on baseline microbiome composition, the specific intervention (diet, probiotic, fiber, medication), stress levels, and individual biology. Sustained habits produce more durable mental health benefits than brief or intermittent changes.